In a little over a month, I will be walking across the graduation stage to shake the hand of the university president and receive my undergraduate diploma. There's no doubt that I have learned a lot. However, when I stop and think about how only one more year of didactic education stands between me and clinical practice as a Physician Assistant, I develop doubts about whether I have learned even a fraction of what is necessary. I mean, really... How can only 12 more months of education prepare me to be clinic ready?
This concern of mine had never been verbalized, but, from what I learned at the clinic last week, one may have thought I had, and someone was trying to answer them:
This concern of mine had never been verbalized, but, from what I learned at the clinic last week, one may have thought I had, and someone was trying to answer them:
Remember the Basics
... was the theme those answers carried.
A patient was being seen at Oasis a few days after slipping and falling on the ice. The swelling in her wrist was substantial and there was a purple/black color that encompassed her wrist. As Andy Booth, PA-C and I entered the exam room we addressed the question, "Is my wrist broken?"
Andy began by asking questions that led to a very detailed, mental image of the patients fall, as well as the pain that was associated with its injuries. Most of the time, I feel as if there are a specific set of questions that practitioners are taught, as if there is a page in a textbook somewhere that says "Questions to Ask if Your Patient has Slipped on the Ice:", but, in reality, Andy was just trying to use basic physics to understand where the impact most likely occurred to better isolate where injuries may be present.
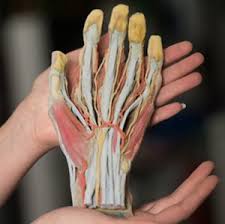
Next, Andy began his examination. He palpated, from the proximal to distal portion of the forearm/hand, checking the ulnar and radial styloid processes followed by each bone of the hand (lunate, scaphoid, pisiform, triquetral, capitate, trapezoid, and trapezium), and as he did, he was taking note of which areas cause the patient to display expressions of pain or discomfort.
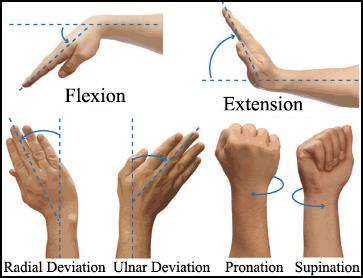
Sure, this could have been a lot easier with an X-ray, but when you are working with an underserved population, you don't always have access to those luxuries. So after palpating it seemed as if Andy had an idea as to which bone may have been affected, and he continued by asking the patient to perform a series of flexion/extension range of motion exercises. Once again, I felt the urge to take notes, but when I tried my best to predict which exercise he was going to request next, I wasn't that far off. I got excited, saying to myself
A patient was being seen at Oasis a few days after slipping and falling on the ice. The swelling in her wrist was substantial and there was a purple/black color that encompassed her wrist. As Andy Booth, PA-C and I entered the exam room we addressed the question, "Is my wrist broken?"
Andy began by asking questions that led to a very detailed, mental image of the patients fall, as well as the pain that was associated with its injuries. Most of the time, I feel as if there are a specific set of questions that practitioners are taught, as if there is a page in a textbook somewhere that says "Questions to Ask if Your Patient has Slipped on the Ice:", but, in reality, Andy was just trying to use basic physics to understand where the impact most likely occurred to better isolate where injuries may be present.
Next, Andy began his examination. He palpated, from the proximal to distal portion of the forearm/hand, checking the ulnar and radial styloid processes followed by each bone of the hand (lunate, scaphoid, pisiform, triquetral, capitate, trapezoid, and trapezium), and as he did, he was taking note of which areas cause the patient to display expressions of pain or discomfort.
Sure, this could have been a lot easier with an X-ray, but when you are working with an underserved population, you don't always have access to those luxuries. So after palpating it seemed as if Andy had an idea as to which bone may have been affected, and he continued by asking the patient to perform a series of flexion/extension range of motion exercises. Once again, I felt the urge to take notes, but when I tried my best to predict which exercise he was going to request next, I wasn't that far off. I got excited, saying to myself
Sweet! I knew that one!
...But how?
...But how?
I know it wasn't because I read the "Range of Motion Exercises When Your Patient Fell on the Ice" chapter, but I sure do remember taking a couple semesters of Anatomy. For those of you who are unfamiliar, anatomy class involves more than just identification of bones and muscles: you have to understand the function of each muscle as well as any movements made possible by joints, ligaments, tendons, bones, etc., and students have spent plenty of hours tugging on cadaver tendons to learn them.
Throughout my undergrad courses I've studied basic chemistry, biology, and the health system. I've learned about how the body was constructed (Anatomy), most of how the body works (Physiology), some of how it "breaks" (Pathophysiology), and the most common drugs used to "fix" it (Pharmacology). What I learned made me a whiz at filling in those scantron bubbles, but when a patient walks in and asks if/which bone in her wrist was broken, my studying felt useless. That was, until I see "textbook" uses of these basics in the clinic setting by providers like Andy Booth.
As I sit and write this blog, I am recalling the countless teachers throughout my educational career that have stressed the importance of understanding vs. rogue memorization, and I guess this would be the perfect example. Now I am still very aware of my need to participate in that 12 more months of didactic coursework mentioned above, but I feel better knowing that this one remaining year does not have to be responsible for teaching me everything there is to know about being a clinician. Rather, my graduate school professors will create a capable health care provider out of me by helping me transition the information I already know from the bubble-sheet to the patient, adding important details along the way.
So when I walk across that stage on April 25 with my Bachelors, I can do so with confidence, because I know that I have been adequately equipped with the basics that I need to be developed into a great clinician.
As I sit and write this blog, I am recalling the countless teachers throughout my educational career that have stressed the importance of understanding vs. rogue memorization, and I guess this would be the perfect example. Now I am still very aware of my need to participate in that 12 more months of didactic coursework mentioned above, but I feel better knowing that this one remaining year does not have to be responsible for teaching me everything there is to know about being a clinician. Rather, my graduate school professors will create a capable health care provider out of me by helping me transition the information I already know from the bubble-sheet to the patient, adding important details along the way.
So when I walk across that stage on April 25 with my Bachelors, I can do so with confidence, because I know that I have been adequately equipped with the basics that I need to be developed into a great clinician.

 RSS Feed
RSS Feed